Psilocybin Cluster Headache: Research, Trials & Relief
Posted under: Psilocybin Science & News

Psilocybin Science News · April 2026 · 9 min read
Psilocybin cluster headache treatment sounds radical. But for more than two decades, people with cluster headache — widely regarded as the most painful condition known to medicine — have been quietly using magic mushrooms to stop their attack cycles. They did this long before any clinical trial existed. Now, science is finally catching up. A new Australian study called the PEACE trial is about to test this approach in a funded, rigorous setting for the first time in the Southern Hemisphere.
At Magic Mushrooms Shop, we know many customers who use psilocybin mushrooms for cluster headache relief — and many of them report promising results. We always encourage you to do this together with a doctor or therapist and not to self midicate. In this article we explain what the research shows, what the PEACE trial is testing, and why this matters to millions of people with few other options.
What Is Cluster Headache — and Why Are Psilocybin Users Paying Attention?
Cluster headache is not a type of migraine. It is its own neurological condition. The pain is extreme and one-sided, often described as a hot poker or a screwdriver pushed into one eye. Attacks last between 15 minutes and 3 hours, and during a cluster period they can happen several times a day, for weeks or months in a row.
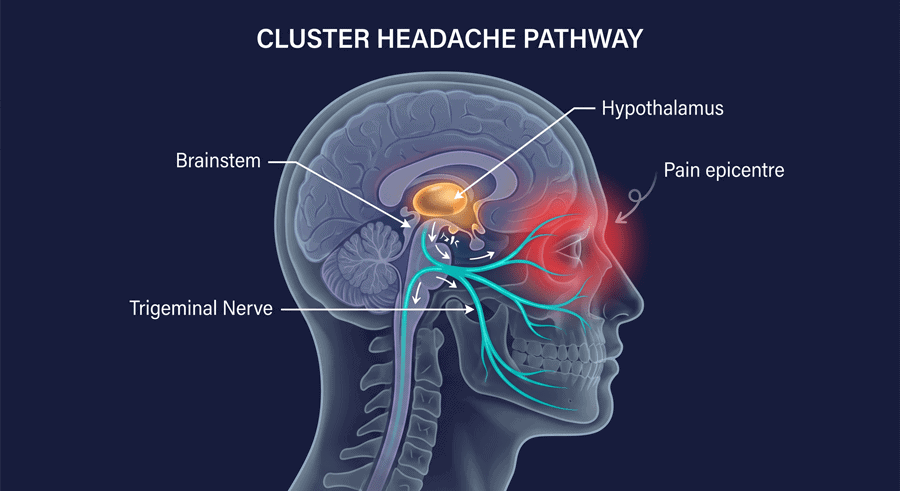
The condition is sometimes called the “suicide headache” because the pain is so severe that some people have considered ending their lives during an active cycle. The hypothalamus — the part of the brain that controls body rhythms — is thought to be the origin of the problem. Attacks often follow a clock-like pattern and come more often in spring and autumn. The trigeminal nerve, the largest nerve in the skull, fires during each attack and creates the intense pain in the face and eye area.
Episodic vs. Chronic Cluster Headache: an Important Difference for Psilocybin Treatment
There are two forms, and the difference matters when thinking about psilocybin as a treatment:
| Type | Pattern | Remission | How common |
|---|---|---|---|
| Episodic | Cluster periods of weeks to months, then complete pain-free intervals | Yes — months to years pain-free between cycles | ~80–85% of patients |
| Chronic | Attacks for more than 12 months without a break longer than 3 months | Minimal or none | ~15–20% of patients |
For episodic patients, psilocybin is typically used at the start of a cluster cycle — ideally during a remission — to prevent or shorten the next bout. For chronic patients, who have no remission windows, timing is harder and ongoing use may be needed. Early research suggests episodic patients respond more reliably. But there are reports of chronic patients reverting to the episodic pattern after psilocybin — a remarkable outcome if confirmed in larger studies.
Important: Cluster headache is a serious neurological condition. Always speak with a neurologist or headache specialist before using psilocybin. It is not suitable for people with a personal or family history of psychosis, certain heart conditions, or those taking SSRIs, MAOIs, or triptans. See our full guide on contraindications and safety.
Patients Found the Answer Before the Scientists Did
The story of psilocybin and cluster headache does not begin in a lab. In the early 2000s, a patient named Bob Wold discovered almost by accident that magic mushrooms could stop a cluster cycle that no prescription medicine had touched. He shared his experience online. Others tried it. The same pattern kept appearing. By 2006, enough patients had found relief that a nonprofit called Clusterbusters was founded to share harm-reduction guidance and push for clinical research.
The method patients use is called a “pulse regimen”: three low doses spaced roughly five days apart, taken either at the start of a cluster period or during remission to head off the next cycle. A 2022 systematic review in Current Pain and Headache Reports confirmed that psilocybin was one of the most consistently reported effective preventive treatments in cluster headache patient surveys — ahead of many approved medications.
What Clinical Research Shows About Psilocybin for Cluster Headache
Controlled trials have been slow because psilocybin is a controlled substance in many countries. But the studies that exist tell a consistent story.
Yale University: the First Controlled Trial (2017–2024)
Dr Emmanuelle Schindler at Yale School of Medicine ran the first randomised, double-blind, placebo-controlled trial of psilocybin in cluster headache. Sixteen patients received three doses of psilocybin (10 mg per 70 kg bodyweight) at five-day intervals, or a placebo. The study was too small to reach statistical significance, but individual results were encouraging, and the treatment caused no serious side effects.
A 2024 follow-up study in Headache repeated the pulse regimen in the same group. This time the results were significant. Attack frequency dropped from an average of 18.4 attacks per week at the start to 9.8 per week after treatment — a reduction of roughly 50% (p = 0.013). Importantly, patients who had not responded the first time still benefited the second time. That tells us that a lack of early response is not a reason to give up.
Denmark: Open-Label Study in Chronic Cluster Headache
A Danish open-label study followed 10 people with chronic cluster headache through a three-week psilocybin pulse. Attack frequency fell by an average of 31%. One patient went 21 weeks completely pain-free — the longest documented remission from psilocybin cluster headache treatment in any published study. Individual results varied widely, which likely reflects differences in timing, whether the condition was episodic or chronic, and individual brain chemistry.
Key Discovery: the Psychedelic Experience Is Not the Point
A 2025 paper in Neurology answered an important question: do patients need to have a full psychedelic experience for psilocybin to help their headaches? The answer is no. In pooled data from Yale migraine and cluster headache trials, headache improvement was completely independent of how intense the psychedelic effect was. This suggests psilocybin works directly on the neurological system driving cluster headache — not through psychological insight. It also opens the door to future non-hallucinogenic versions of psilocybin that could treat headaches without causing any altered state. To understand how psilocybin acts in the brain, read our guide on psilocybin and neuroplasticity.
How does it work? The leading theory is that psilocybin activates serotonin 5-HT2A receptors in the hypothalamus and trigeminal system. This may “reset” the disrupted body-clock and pain-signalling loops that cause cluster cycles. Psilocybin also promotes the growth of new neural connections, which may help the brain break out of established pain patterns. Learn more about how psilocybin works.
The PEACE Trial: the Biggest Psilocybin Cluster Headache Study Yet
The PEACE trial (Psilocybin Efficacy and Acceptability on Cluster Headache Episodes) is led by Dr Faraidoon Haghdoost at The George Institute for Global Health, UNSW Sydney. The Australian federal government awarded AU$800,000 through the Medical Research Future Fund (MRFF). It is the first new approved clinical trial for cluster headache in Australia in at least twenty years.
The trial is a randomised, placebo-controlled pilot study with 40 cluster headache patients. They will receive either 10 mg of oral psilocybin once a week for four weeks, or a placebo. The main goal is to find out whether this weekly low-dose approach can prevent or significantly reduce attacks. The team will also collect safety data and measure how acceptable the treatment is to patients — building the base for a larger study if results are positive.
A George Institute survey of more than 200 Australian cluster headache patients showed that only 6% felt their current treatment was fully working. One in four had never seen a headache specialist — only a GP. Yet 62% said they would join a clinical trial, and within that group 66% were open to psilocybin specifically. These figures were published in Headache: The Journal of Head and Face Pain.
“If the PEACE findings are positive, we hope to do larger trials with the aim of providing an effective, evidence-based treatment option using affordable generic psilocybin for those enduring cluster headache.”
— Dr Faraidoon Haghdoost, The George Institute for Global Health, UNSW Sydney
Other Serious Headache Conditions: What Does Psilocybin Research Show?
Cluster headache gets the most research attention, but psilocybin is also being studied for other debilitating headache and pain conditions. Here is where the science currently stands.
Migraine
Migraine affects roughly 15% of the world’s population and is the leading cause of disability in people under 50. In a 2020 Yale proof-of-concept study, a single low psilocybin dose cut weekly migraine days by about 50% versus placebo, with effects lasting two weeks. A 2025 follow-up RCT with 18 patients found both single-dose and two-dose psilocybin regimens reduced migraine days by roughly 60% over eight weeks. A large 2025 population study in the Journal of Psychopharmacology found that people who had ever used classic psychedelics had 25% lower odds of reporting frequent bad headaches — a striking signal that deserves further investigation.
SUNHA (Short-Lasting Unilateral Neuralgiform Headache Attacks)
SUNHA is a rare condition with very brief but extremely severe one-sided attacks, often dozens of times a day. A 2024 open-label phase Ib study of ascending psilocybin doses in 10 SUNHA patients found no clear reduction in attack frequency. However, many patients reported a qualitatively changed relationship with their pain — suggesting that psychological dimensions of SUNHA may matter more than in cluster headache, and that future studies need a different design.
Fibromyalgia and Widespread Chronic Pain
Fibromyalgia causes widespread pain, fatigue, sleep problems, and brain fog, and responds poorly to most drugs. A 2025 open-label pilot in Frontiers in Pain Research gave five fibromyalgia patients two psilocybin sessions (15 mg and 25 mg) with psychotherapy support. Pain severity fell by an average of 2.3 points and pain interference by 9.4 points — both clinically meaningful changes. A separate 2025 preclinical study in Nature Neuroscience from the University of Pennsylvania showed that a single psilocybin dose rapidly and durably reversed pain sensitivity in two animal chronic pain models, with effects lasting at least 12 days. That points to a real analgesic mechanism, not just a mood improvement.
Neuropathic Pain
Neuropathic pain — caused by damaged or dysfunctional nerves — affects hundreds of millions of people and is notoriously hard to treat. The PEACE-PAIN trial (a separate study from the PEACE cluster headache trial) is planned to test psilocybin-assisted therapy specifically for chronic neuropathic pain. A 2024 preference study found that 76.9% of neuropathic pain patients were willing to take part — a strong sign of how much people in this community need better options.
| Condition | Best evidence to date | Current status |
|---|---|---|
| Cluster headache | ~50% reduction in attacks after repeat pulse (Yale, 2024) | PEACE RCT recruiting, Australia 2026 |
| Migraine | ~60% fewer migraine days over 8 weeks (Yale, 2025) | Larger trials needed |
| SUNHA | No clear frequency reduction; qualitative pain shifts reported | Refined studies recommended |
| Fibromyalgia | Meaningful pain reduction in pilot (Frontiers in Pain Research, 2025) | Larger controlled trial needed |
| Neuropathic pain | Durable pain reversal in animal models (Penn, 2025) | PEACE-PAIN trial planned |
Why Standard Treatments Are Not Enough
Cluster headache medicine has not changed much in decades. For acute attacks, the main options are high-flow oxygen (effective in roughly 70% of attacks), sumatriptan injections, and nasal spray triptans. For prevention, verapamil is the standard choice, with lithium added for chronic cases. In 2019, Emgality (galcanezumab) became the first drug specifically approved for episodic cluster headache, cutting attacks by about half in most trial participants. But in real life, only 6% of patients say their treatment works completely. The side effects of verapamil and lithium are significant and require regular blood monitoring. For chronic cluster headache especially, the treatment gap is large — and that is precisely why psilocybin research matters so much right now.
Drug interaction alert: Psilocybin interacts with serotonin-affecting medications including SSRIs, SNRIs, MAOIs, and triptans like sumatriptan. If you take any of these, speak with your doctor before considering psilocybin. Read our full guide to magic mushroom safety and contraindications.
What We See at Magic Mushrooms Shop
Over the years, we have built relationships with many customers who use our products specifically to manage cluster headache. Their stories are consistent: most describe a real reduction in attack frequency, some report a full break in a cluster cycle, and a number have kept that benefit going through occasional use. These experiences match the patterns seen in patient surveys and early clinical trials. We are proud to be part of a community that found this answer before the science arrived to confirm it.
We always recommend working with a doctor or therapist who understands your full health picture. Know your set and setting. Have a trusted trip sitter. Approach dosage carefully. This applies to everyone, including those using psilocybin for a medical reason.
Curious about growing your own psilocybin mushrooms at home?
Read our complete grow kit guide →
What Comes Next
The PEACE trial is a pilot with 40 participants. Its job is to generate reliable safety and effect-size data, not to deliver a final verdict. If the results are positive, the George Institute plans to run a larger multi-centre trial. Australia is well-placed to move quickly — it became the first country to allow psychiatrists to prescribe MDMA and psilocybin in 2023, so the regulatory path from a positive trial to clinical access is shorter there than almost anywhere else in the world.
For the global cluster headache community — people who have used psilocybin quietly for over two decades, often without medical support and often in legal grey areas — the PEACE trial means something beyond science. It means recognition. It means that what they discovered on their own is now being taken seriously. We will follow the results and report back. Keep an eye on our psilocybin research news for updates.


April 27, 2026