Mushrooms and the Mind: How Psilocybin Works in the Brain
Publicado de: Psilocybin Science & News

How psilocybin works in the brain — default mode network, serotonin, and neuroplasticity explained (2026 Update)
When people describe a magic mushroom experience, they often say something shifted in how they think, how they see themselves, or how connected they feel to the world. These are not random impressions. Researchers are now finding clear biological reasons for them. The science of mushrooms and the mind has developed remarkably fast over the past decade, and the results are genuinely interesting — even if you have no intention of ever trying psilocybin.
This cornerstone guide explains what actually happens inside the brain when psilocybin is present, from its first chemical interaction right through to the longer-term changes in neural wiring that researchers are now studying closely.
In this guide: A thorough, science-backed look at how psilocybin interacts with serotonin receptors, quiets the default mode network, and promotes neuroplasticity in the human brain.
We cover the key mechanisms in plain language — no neuroscience degree needed.
| Active compound | Psilocybin (converted to psilocin in the body) |
| Primary receptor target | 5-HT2A serotonin receptors |
| Key brain network affected | Default Mode Network (DMN) |
| Duration of acute effects | 4–6 hours |
| Research status (2026) | Phase 2/3 clinical trials ongoing worldwide |
From Mushroom to Molecule: What Is Psilocybin?
Psilocybin is a naturally occurring compound found in over 200 species of fungi — the most widely studied being Psilocybe cubensis. In its raw form, psilocybin is actually a prodrug. That means the body must convert it into something else before it becomes active. The enzyme alkaline phosphatase in your gut and liver strips away a phosphate group, turning psilocybin into psilocin — the molecule that actually crosses the blood-brain barrier and goes to work.
This conversion happens relatively quickly, usually within 20 to 40 minutes of ingestion. Once psilocin is in the bloodstream and reaches the brain, it begins mimicking a neurotransmitter the brain already knows well: serotonin. To understand what happens next, it helps to know a little about how serotonin itself works.
You can read more about the basics of magic mushroom chemistry in our guide to what magic mushrooms are and how they differ from other fungi.
Serotonin, Receptors, and the 5-HT2A Connection
Serotonin is one of the brain's most important signalling molecules. It plays a role in mood regulation, appetite, sleep, memory, and social behaviour. The brain has at least 14 different types of serotonin receptors, but the one most relevant to psilocybin is the 5-HT2A receptor.
Psilocin binds to 5-HT2A receptors with high affinity — meaning it fits into them easily and triggers a strong response. However, it activates these receptors in a way that is somewhat different from serotonin itself. This difference in receptor signalling is what researchers call "biased agonism," and it is thought to be part of why psilocybin produces such unusual perceptual and cognitive effects rather than simply acting like a serotonin boost.
The 5-HT2A receptors targeted by psilocin are concentrated in the cortex — the outer layer of the brain responsible for higher thinking, perception, and self-awareness. When these receptors are activated at high levels, the normal filtering and organising functions of the cortex become disrupted. Signals that would normally be suppressed start to get through. This is one reason why sensory experiences often feel more vivid and thoughts can feel unusually significant during a psilocybin experience.
Key concept: Psilocin does not simply flood the brain with serotonin — it mimics serotonin but activates receptors differently, producing effects that serotonin itself does not create.
The Default Mode Network: Your Brain's Autopilot
One of the most important discoveries in modern neuroscience is the default mode network (DMN) — a set of interconnected brain regions that become active when you are not focused on a specific task. The DMN is associated with self-referential thinking: daydreaming, ruminating, planning, and the ongoing narrative of "I" that most people experience as their sense of self.
In healthy individuals, the DMN switches on during rest and switches off during focused activity. However, in people with depression, anxiety, and PTSD, the DMN can become overactive and rigid — constantly replaying the same thoughts, fears, and self-critical narratives. Researchers at Imperial College London have described this as a kind of "neural rut."
How Psilocybin Disrupts the DMN
Neuroimaging studies using fMRI have shown that psilocybin significantly reduces activity in the DMN. In a landmark 2012 study published in PNAS by Carhart-Harris et al., participants given psilocybin showed measurable decreases in blood flow to key DMN regions — particularly the medial prefrontal cortex and the posterior cingulate cortex. These regions are associated with self-referential processing and rumination.

As the DMN quietens, the normal boundaries between different brain networks become less rigid. Brain regions that do not usually communicate with each other begin exchanging signals. This is sometimes called "hyper-connectivity" — and it is associated with the unusual, fluid quality of thought that people often describe during a mushroom experience. Connections form between sensory areas and conceptual areas that normally operate independently, which may explain phenomena like synesthesia (perceiving sounds as colours, for example).
Importantly, once the psilocybin has cleared, the DMN does not simply return to its exact previous state. Studies suggest it re-emerges with less rigidity — and this loosening of fixed patterns may be central to the therapeutic potential of psilocybin. You can explore more about the psychological dimension of these experiences in our post on mushrooms and the mind.
Neuroplasticity: Rewiring the Brain
Perhaps the most exciting area of current research is the effect of psilocybin on neuroplasticity — the brain's ability to form new connections and reorganise existing ones. For a long time, scientists believed that the adult brain was relatively fixed in its structure. We now know this is not true, but we also know that different experiences promote different degrees of plasticity.
Laboratory studies have shown that psilocybin promotes the growth of new dendritic spines — the tiny protrusions on neurons through which signals pass between cells. A 2021 study published in Neuron by researchers at Yale University found that a single dose of psilocybin in mice produced a 10% increase in the size and density of dendritic spines in the frontal cortex, and that these structural changes persisted for at least a month.
This is significant because reduced dendritic spine density is associated with stress, depression, and certain psychiatric conditions. The ability of psilocybin to reverse or counteract these structural changes — rapidly and with apparently lasting effect — is one reason why it has attracted so much clinical interest.
BDNF and the Growth Factor Connection
Psilocybin also appears to increase levels of BDNF (brain-derived neurotrophic factor), a protein that supports the survival of existing neurons and encourages the growth of new ones. BDNF is often described as a kind of "fertiliser" for the brain. Low BDNF levels have been linked to depression, and conventional antidepressants also work in part by raising BDNF — but they typically take weeks to do so. Psilocybin may achieve similar or greater effects much more rapidly.
This fast-acting neuroplasticity could explain why some people report lasting changes in mood, habit, and outlook after even a single experience. The brain, it seems, becomes temporarily more receptive to new patterns of thinking — and what you do with that window matters. This is one reason why guided settings and integration practices have become a focus in clinical research.
Entropy and the Unshackling of Fixed Thought
Researcher Robin Carhart-Harris has proposed a theoretical framework called the entropic brain hypothesis. In brief, this model suggests that the brain normally operates in a constrained, low-entropy state — running on familiar, well-worn patterns of thought and perception. Depression and anxiety can push this entropy even lower, locking a person into repetitive negative loops.
Psilocybin temporarily increases neural entropy — in other words, it broadens the range of brain states available to the person. This increased entropy is not chaos; it is more like a brief period of heightened flexibility, during which the brain becomes capable of making new connections and experiencing genuinely novel perspectives.
After the acute experience, if conditions are right, the brain can settle back into a lower-entropy state that is nonetheless different from — and healthier than — the one it occupied before. This is the mechanistic foundation for the idea that psilocybin might help people break out of rigid thought patterns, whether those patterns take the form of depression, addiction, or simply a stuck sense of self.
The Serotonin–Psilocybin Link and Antidepressants
One question that often arises is: if psilocybin works on serotonin receptors, what happens if someone is already taking SSRIs (selective serotonin reuptake inhibitors)? SSRIs increase serotonin availability by blocking its reabsorption, but they also downregulate (reduce the sensitivity of) 5-HT2A receptors over time.
This is clinically relevant because people who take SSRIs long-term may find that psilocybin has a noticeably reduced effect. Current clinical trials are actively studying this interaction, and some researchers have suggested a supervised taper before psilocybin-assisted therapy — always under medical supervision. This highlights how interconnected the serotonin system is, and why understanding the receptor-level mechanisms matters for safe and effective use.
Important: Never stop or reduce prescribed medication without consulting your doctor. The interaction between SSRIs and psilocybin is a matter for medical supervision, not self-experimentation.
Integration: What Happens After
The neuroscience strongly suggests that psilocybin opens a window — but what happens within and after that window shapes the outcome. Research in therapeutic settings consistently shows that preparation and integration work (processing the experience through conversation, reflection, or creative expression) significantly improves outcomes.
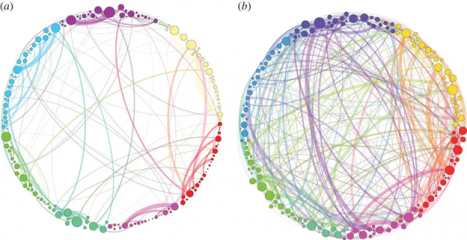
The temporary increase in neuroplasticity means the brain is more responsive to new input during and after a psilocybin experience. People who use this period intentionally — through therapy, journaling, meditation, or meaningful conversations — appear to get more durable benefits than those who do not. This is why responsible clinical approaches always pair psilocybin with structured support.
For a closer look at how to approach a psilocybin experience thoughtfully, our guide to set and setting is a good starting point. You might also find our post on turning a trip into a ceremony useful for thinking about intentional framing.
Where the Research Stands in 2026
As of 2026, psilocybin-assisted therapy is in Phase 2 and Phase 3 clinical trials for treatment-resistant depression, PTSD, alcohol use disorder, and end-of-life anxiety at major research institutions including Imperial College London, Johns Hopkins University, and NYU. Australia became the first country to formally authorise psychiatrist-supervised psilocybin therapy in 2023, a significant regulatory milestone.

The research base is growing quickly. Each new study adds detail to the neurological picture — refining our understanding of which brain regions are most affected, which patient populations benefit most, and what conditions maximise the therapeutic potential of these experiences. The fundamental picture, however, is already remarkably clear: psilocybin produces measurable, lasting changes in brain structure and function, and those changes align with what people describe in their experiences.
For a broader view of psilocybin's therapeutic applications, see our dedicated post on the healing power of magic mushrooms.
Curious about magic mushrooms? Explore our full range of magic mushroom grow kits — carefully selected for quality and reliability.
Note: If you are suffering from a mental illness and are curious about using psilocybin or any other psychedelic therapy, please consult one of the relevant medical authorities first. Do not self-prescribe — it is vital to have the right support and guidance when using psychedelics as medicine.


March 23, 2026