Ketamine Assisted Therapy 101
Publié sous: Psilocybin Science & News

Ketamine started as a surgical anesthetic. Today, it is one of the most promising tools in mental health treatment. If you struggle with treatment-resistant depression, PTSD, or chronic anxiety, ketamine-assisted therapy may offer the rapid relief you have been looking for.
In this guide, you will learn what ketamine is, how therapy sessions work, and what you need to know before you begin.
| Originally approved | 1970 (as an anesthetic) |
| First depression study | 2000 (Yale / Berman et al.) |
| FDA-approved nasal spray | Spravato (esketamine) – 2019 |
| Common methods | IV infusion, intramuscular injection, lozenge, nasal spray |
| Typical session length | 40–60 minutes |
| Cost range (full course) | $3,300–$27,300 depending on method and insurance |
What Is Ketamine?
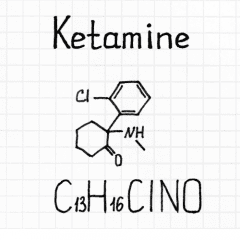
Ketamine is a dissociative anesthetic and painkiller. Doctors have used it in surgery and veterinary medicine since the 1970s. In recent years, however, researchers discovered it can also improve mental health — and fast.
So how does it work? Ketamine blocks NMDA receptors in the brain. This action increases glutamate, a neurotransmitter that helps the brain form new neural connections. As a result, it boosts neuroplasticity and can interrupt the ruminative thought patterns linked to depression and anxiety.
Unlike traditional antidepressants that target serotonin, ketamine works through the glutamate system. Because of this different pathway, some patients feel relief within hours instead of weeks. That rapid action makes it especially valuable for people with treatment-resistant depression, PTSD, OCD, suicidal ideation, and chronic pain.
The History of Ketamine

Ketamine was first synthesised in 1962 by Parke-Davis (now part of Pfizer). The goal was to create a safer alternative to phencyclidine (PCP) with fewer hallucinogenic side effects. The FDA approved it as an anesthetic in 1970, and the U.S. military soon adopted it as a battlefield anesthetic during the Vietnam War.
During the 1970s and 1980s, recreational misuse of ketamine grew. This led to its classification as a Schedule III controlled substance. However, researchers at Yale University noticed something remarkable in the early 1990s. Patients recovering from surgery reported feeling emotionally "lighter" after receiving ketamine.
In 2000, the first placebo-controlled clinical trial confirmed that a low dose of ketamine could rapidly reduce depression symptoms. Studies between 2000 and 2006 built on that finding. Then, in 2019, the FDA approved Spravato (esketamine nasal spray) specifically for treatment-resistant depression. Today, hundreds of studies worldwide continue to explore ketamine's mental health applications.
What Is Ketamine-Assisted Therapy?
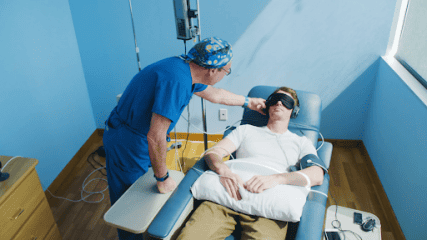
Ketamine-assisted therapy (KAP) combines ketamine with psychotherapy. During a session, a clinician administers a low dose of ketamine — usually through an IV — while you relax in a comfortable setting. Some practitioners also offer sleep masks or headphones to deepen the experience.
The ketamine creates a dissociative state that can lower emotional defences. In this state, therapists help you process difficult thoughts, memories, and patterns that talk therapy alone may not reach. Many people describe feeling more open and less "stuck" during these sessions.
On a neurological level, ketamine increases synaptic plasticity. It activates the glutamate system and helps the brain build new neural pathways. Abnormal glutamate levels are linked to depression, so restoring balance in this system can produce rapid mood improvements. Additionally, glutamate plays a role in pain perception, which is why ketamine also helps with chronic pain.
Results vary from person to person. Some people notice improvement after a single session, while others need a full course of treatment. The number of sessions depends on your condition, your response, and your therapist's recommendations.
How Does Ketamine Feel?
The experience depends on the dose. At therapeutic (subanesthetic) doses, most people report a range of effects. Here are the most common ones:
However, some people also experience temporary side effects. These can include nausea, dizziness, blurred or double vision, confusion, and poor coordination. These effects are usually short-lived and fade once the session ends.
Tip: Listening to calming music during your session can help guide the experience in a positive direction and reduce any discomfort.
Methods of Administration
Ketamine can be delivered in several ways. Each method has its own onset time, duration, and cost profile.
⚠️ Important: The FDA has raised concerns about compounded ketamine prescribed online without adequate medical oversight. Always ensure your treatment is supervised by a licensed professional.
How to Prepare for a Session

Good preparation makes a real difference. Follow these steps to get the most out of your ketamine therapy session.
Fast Before Your Session
Avoid eating for at least 6–8 hours before your appointment. Also limit fluids in the hours beforehand. This helps your body absorb the ketamine properly and reduces the chance of nausea.
Wear Comfortable Clothing
Choose loose, relaxed clothing that allows you to move and breathe easily. You will be sitting or lying down for the duration, so comfort is key.
Set Your Intention
Take a few moments to reflect on why you are pursuing this treatment. Are you seeking relief from depression? Processing trauma? Gaining new insights? A clear intention helps guide the experience.
Prepare a Playlist
Music can shape your session in powerful ways. Create a calming playlist and bring headphones to block out external distractions. Many clinics also provide their own curated playlists.
Practise Mindfulness
A short meditation or breathing exercise before your session can calm your nervous system. Even five minutes of deep breathing helps you arrive in a more receptive and open state of mind.
Tip: Get a good night's rest and eat a light, nutritious meal the day before. Avoid alcohol and recreational drugs for at least 24 hours prior.
Where Is Ketamine Therapy Legal?
Ketamine has been approved as an anesthetic since the 1970s. Using it to treat psychiatric conditions is considered "off-label." This means a licensed doctor can legally prescribe it, even though it is not specifically approved for that use.
The key exception is Spravato (esketamine nasal spray). The FDA approved it in 2019 specifically for treatment-resistant depression. In the United States, ketamine is a Schedule III controlled substance, so clinics must hold DEA registrations and follow strict storage and monitoring rules.
Legal status varies around the world. In the UK, for example, the government proposed reclassifying ketamine from Class B to Class A in January 2025. In most countries, medical use under professional supervision remains legal. However, regulations for at-home or telehealth-based ketamine therapy differ significantly by region. Check this resource to see if therapy is available where you live.
Safety, Risks, and Cost
When administered at low doses in a supervised clinical setting, ketamine therapy has a favourable safety profile. Most side effects — such as nausea, dizziness, and temporary dissociation — are mild and short-lived.
However, there are important risks to be aware of:
⚠️ Do not self-medicate with ketamine. It can cause serious physical and psychological side effects. Always work with a licensed medical professional.
What Does It Cost?
Ketamine therapy costs vary widely depending on the method, location, and insurance coverage. Here is a general overview for a full treatment course in the United States:
| Method | Self-Pay (Full Course) | With Insurance |
|---|---|---|
| Intramuscular injection | $3,300–$6,050 | Rarely covered |
| IV infusion | $4,675–$13,500 | Rarely covered |
| Spravato nasal spray | $16,800–$27,300 | $2,940–$9,450 |
Spravato is most likely to be covered by insurance because it carries FDA approval. IV and injection-based therapies are typically out-of-pocket expenses. Some clinics offer payment plans to make treatment more accessible.
Is Ketamine Therapy Right for You?
Ketamine-assisted therapy is not a magic cure. However, for people who have not responded to traditional antidepressants, it offers a scientifically backed alternative with rapid results. Research continues to grow — a 2025 University of Florida study found that over 80% of PTSD patients reported better sleep, less anxiety, and fewer trauma triggers after ketamine treatment.
If you are considering this path, start by consulting a qualified mental health professional. They can assess whether ketamine therapy suits your specific situation and guide you toward a safe, supervised treatment plan.
⚠️ Note: If you are suffering from a mental illness and are curious about ketamine, psilocybin, or any other psychedelic therapy, please consult a medical professional first. Do not self-prescribe. The right support and guidance are vital when exploring psychedelics as medicine.
Curious about the therapeutic potential of psychedelics?
Explore the Magic Mushrooms Shop for trusted products, grow kits, and educational resources.


Février 12, 2024